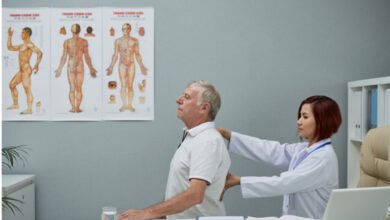
7 Signs Your Healthcare Organization Needs Custom EHR Integration
Healthcare in the United States has undergone a massive digital transformation over the past decade. From small clinics to sprawling hospital networks, electronic health record (EHR) systems have become the backbone of how patient data is captured, stored, and shared. The push toward digitization was supposed to make everything smoother from faster access to patient histories, fewer paper trails, and better coordination between care teams.
But here’s the thing, for many organizations, that promise hasn’t fully materialized.
Instead of streamlining care, a lot of EHR systems have quietly become silos. They store mountains of data, sure, but getting that data to talk to other systems? That’s where things start to break down. Labs, imaging platforms, billing software, telehealth tools all generate critical information, yet they often operate in their own bubbles. The result is a fragmented digital environment where clinicians, administrators, and patients all feel the friction.
And it’s not only inconvenient but also costly. Operational inefficiencies, billing errors, compliance risks, and clinician burnout are just the tip of the iceberg when your systems aren’t working in sync.
So how do you know if your organization has reached that tipping point?
In this blog, we’re breaking down seven telltale signs that your healthcare organization needs custom EHR integration. If any of these hit close to home, it might be time to rethink how your systems connect, and explore the custom EHR integration benefits that can genuinely transform your operations.
Sign 1: Clinician Burnout and Click Fatigue
Let’s start with what’s arguably the most human cost of a broken EHR setup — clinician burnout.
If your doctors, nurses, and clinical staff are spending more time clicking through screens than actually caring for patients, that’s a red flag. And unfortunately, it’s incredibly common. Many healthcare professionals report spending a significant portion of their day on documentation and administrative tasks rather than direct patient interaction.
Now, when an EHR system isn’t well-integrated, the problem only gets worse. For example, clinicians end up toggling between multiple platforms—one for charting, another for lab results, and a third for prescriptions—copying and pasting data, or worse, re-entering it manually.
This kind of “click fatigue” isn’t just annoying. It leads to cognitive overload, errors in documentation, and a growing sense of frustration that drives talented people out of the profession. The administrative burden becomes the job, and patient care takes a back seat.
Now imagine the alternative. A custom-integrated EHR environment where workflows are streamlined, for instance, lab results flow automatically into patient charts, AI-assisted tools handle repetitive documentation, and clinicians can access everything they need from a single interface.
That’s not a pipe dream. It’s what thoughtful integration makes possible. When you reduce the number of clicks and screens between a clinician and their patient, you’re not just improving efficiency but instead you’re giving healthcare workers their time (and sanity) back.
Sign 2: No Real-Time Data from Labs and Imaging Systems
Here’s a scenario that plays out in healthcare facilities every single day: a physician orders a lab test or an imaging study, and then… They wait. Not because the test hasn’t been run, but because the results are sitting in a completely separate system that doesn’t communicate with the EHR. Sometimes the results come through via fax. Yes, fax — in an era of cloud computing and AI. Other times, clinicians have to log into a separate portal, track down the report, and manually enter findings into the patient’s chart.
This isn’t just an inconvenience — it’s a patient safety issue. When critical lab values or imaging findings are delayed, clinical decisions get delayed right along with them. A sepsis marker that takes an extra hour to reach a physician’s screen could mean the difference between early intervention and a life-threatening escalation.
The root of this problem?
A lack of real-time interoperability. Your EHR, laboratory information system (LIS), and radiology information system (RIS) are all doing their jobs individually, but they’re not talking to each other in a meaningful, timely way.
This is exactly where modern integration standards like HL7 FHIR (Fast Healthcare Interoperability Resources) come into play. FHIR enables systems to exchange data in real time using standardized APIs, which means lab results, imaging reports, and diagnostic data can flow seamlessly into the EHR the moment they’re available. No fax machines. No portal-hopping. No unnecessary delays.
If your organization is still relying on manual data entry or batch processing to move clinical data between systems, that’s a clear sign you need a more connected integration strategy.
Sign 3: Billing Errors and Revenue Leakage
If there’s one thing that keeps healthcare administrators up at night, it’s revenue leakage — money that walks out the door because of preventable billing errors. And more often than not, those errors trace back to a disconnect between clinical documentation and the billing process.
Here’s how it typically goes wrong. A clinician documents a procedure or diagnosis in the EHR. That information then needs to be translated into billing codes—CPT, ICD-10, HCPCS—and submitted as a claim.
But when the EHR and billing systems aren’t tightly integrated, things get lost in translation. Maybe the documentation is incomplete. Maybe the coder doesn’t have enough clinical context to assign the right code or the claim gets submitted with inaccurate information and comes back denied. Each of these scenarios costs your organization real money.
Claim denials are a massive pain point for healthcare organizations across the country. A significant percentage of claims are denied on the first submission, and reworking those claims eats up staff time, delays reimbursement, and in many cases, the revenue is simply never recovered. The financial impact adds up fast, especially for organizations processing thousands of claims every month.
The fix? An integrated workflow that connects clinical documentation directly to the billing pipeline. When your EHR, coding tools, and practice management system are working together as one cohesive unit, charge capture becomes more accurate, coding aligns with documentation in real time, and claims go out cleaner the first time around. Automated checks can flag inconsistencies before a claim is submitted, reducing denials and the administrative overhead of chasing down corrections. If your billing team spends more time fixing errors than processing clean claims, it’s time to look at integration as a revenue strategy — not just a tech upgrade.
Sign 4: Fragmented Patient Records Across Systems
Think about this from a patient’s perspective for a moment. They see a primary care physician at one clinic, a specialist at another, get bloodwork done at an outside lab, and maybe have a procedure at a hospital across town.
Each of those touchpoints generates data—clinical notes, lab results, medication lists, imaging reports—but that data often lives in completely different systems. And in many cases, none of those systems are aware that the others exist.
Now flip back to the provider’s perspective. A physician is about to make a treatment decision, but they only have a partial picture of the patient’s health history. They can see what happened in their own system, but not the MRI from last month at a different facility, or the medication change made by the specialist two weeks ago. It’s like trying to solve a jigsaw puzzle with half the pieces missing.
This fragmentation isn’t just frustrating but dangerous. Incomplete records can lead to duplicate tests, missed drug interactions, contradictory treatment plans, and a patient experience that feels disjointed and impersonal.
What healthcare organizations truly need is a unified patient view — a single, consolidated record that brings together data from every system, every location, and every provider involved in a patient’s care.
Custom EHR integration makes this possible by synchronizing records across platforms and creating a centralized source of truth. Whether a patient walks into your emergency department or logs into a telehealth appointment, every clinician who touches that patient’s care should have access to the same, complete, up-to-date information. That’s not a luxury — it’s a baseline requirement for delivering safe, coordinated care.
Sign 5: Increasing Compliance and Security Challenges
Healthcare is one of the most heavily regulated industries in the country, and for good reason — patient data is among the most sensitive information out there. Between HIPAA requirements, ONC (Office of the National Coordinator for Health IT) regulations, information blocking rules, and an ever-evolving landscape of state and federal mandates, staying compliant is practically a full-time job.
Now layer in the reality that many healthcare organizations are running on legacy EHR systems — platforms that were built years ago and were never designed to adapt to the pace of regulatory change we see today. These systems are rigid, difficult to update, and often lack the infrastructure needed to support modern security protocols. When a new compliance requirement rolls in, the response is usually a patchwork fix rather than a structural solution. And patchwork doesn’t hold up under audit scrutiny.
The security side of the equation is equally concerning. Healthcare data breaches have been climbing year over year, and organizations with fragmented, poorly integrated systems are more vulnerable. When data flows through disconnected channels—unencrypted emails, unsecured file transfers, or outdated interfaces—the attack surface grows. Every gap between systems is a potential point of failure.
What organizations need is an integration-driven infrastructure that’s built with compliance and security at its core. Custom EHR integration allows you to implement consistent data governance policies across all connected systems, enforce role-based access controls, encrypt data in transit and at rest, and maintain detailed audit trails. More importantly, it gives you the flexibility to adapt quickly when regulations change — without ripping out the foundation. If your compliance team is constantly playing catch-up, or if your IT team dreads every regulatory update, your systems are overdue for a more thoughtful integration approach.
Sign 6: Poor Support for Telehealth and Remote Patient Monitoring
Telehealth went from being a “nice to have” to a necessity almost overnight during the pandemic, and it’s here to stay. Remote patient monitoring (RPM) is right behind it, with wearable devices and home health tools generating a constant stream of patient data like blood pressure readings, glucose levels, heart rate patterns, oxygen saturation, and more. The potential for proactive, data-driven care is enormous.
But here’s the catch! In many healthcare organizations, telehealth platforms and RPM tools operate completely independently from the core EHR. A virtual visit happens on one platform, the notes get stored somewhere else, and the data from a patient’s home blood pressure monitor?
It might live in a third app altogether. The clinician treating that patient has to piece it all together manually, if they even have access to all of it.
This disconnect means valuable patient-generated data is either missed entirely or underutilized. A patient’s blood pressure could be trending upward for weeks, but if that data isn’t flowing into the EHR and triggering alerts, the care team might not catch it until the patient ends up in the emergency room.
The solution is integration — bringing telehealth platforms, RPM devices, patient portals, and the EHR together into one connected ecosystem. When a virtual visit note populates the same chart as an in-person visit, when wearable data feeds directly into the patient record and triggers clinical alerts, and when care teams can see the full picture regardless of where the data originated — that’s when digital health tools actually deliver on their promise. If your telehealth and RPM systems feel like islands disconnected from the mainland, it’s a strong indicator that custom integration should be on your radar.
Sign 7: Your EHR Cannot Scale with Organizational Growth
Growth is supposed to be a good thing. You’re adding new providers, expanding to new locations, launching new service lines — all signs that your organization is thriving. But if your EHR system buckles every time you try to scale, that growth becomes a headache instead of a celebration.
This is a reality many healthcare organizations face. The EHR that worked perfectly fine for a single-location practice starts showing cracks when you add a second or third site. Performance slows down. New departments need custom workflows that the system can’t support without expensive workarounds. Onboarding new providers becomes a drawn-out process because the system wasn’t designed to handle that kind of expansion. And before you know it, your technology is the bottleneck holding back your growth strategy.
Legacy EHR systems, in particular, tend to struggle here. They were often built as monolithic platforms, one big block of software that does everything in one way. Adding new capabilities or connecting new tools requires major development effort, if it’s even possible at all. You end up locked into a system that can’t keep up with the pace of your organization.
This is where a scalable, API-driven integration architecture becomes essential. Instead of relying on a single system to do everything, you build an ecosystem where specialized tools can be plugged in and connected through APIs. Need to add a new specialty clinic? Integrate it. Rolling out a new patient engagement platform? Connect it. Expanding into a new state with different regulatory requirements? Adapt without starting from scratch. A well-integrated architecture gives you the flexibility to grow on your terms — not on the terms dictated by your EHR vendor’s limitations. If scaling up feels like an uphill battle, your integration strategy needs a serious upgrade.
The Bigger Picture: Why Integration Matters Now
If you’ve recognized your organization in even one or two of the signs above, you’re not alone — and the issue is bigger than any single pain point.
The healthcare industry is moving away from the era of standalone systems. The future belongs to connected ecosystems — environments where data flows freely, securely, and intelligently between every system involved in patient care. It’s no longer enough to have a good EHR. You need that EHR to play nicely with your labs, your billing system, your telehealth platform, your RPM devices, your patient portal, and whatever new tool comes along next year.
And then there’s the AI factor. Artificial intelligence and machine learning are rapidly becoming integral to healthcare — from predictive analytics and clinical decision support to automated documentation and population health management. But here’s the kicker: AI is only as good as the data it can access. If your data is siloed, fragmented, or inconsistent, your AI initiatives will fall flat before they even get started. Integration is the foundation that makes AI in healthcare viable.
Interoperability isn’t just a technical buzzword anymore — it’s a strategic imperative. Organizations that invest in custom EHR integration today are positioning themselves to be more agile, more efficient, and more resilient in the face of whatever changes the healthcare landscape throws their way. The custom EHR integration benefits go far beyond fixing today’s problems — they’re about building the infrastructure for tomorrow’s opportunities.
This isn’t about ripping and replacing your entire tech stack. It’s about connecting what you have, filling the gaps that matter most, and building a digital foundation that can evolve with your organization.
Conclusion
The seven signs we’ve covered in this blog—clinician burnout, delayed lab and imaging data, billing errors, fragmented patient records, compliance struggles, disconnected telehealth tools, and scalability limitations—might seem like separate problems on the surface. But dig a little deeper, and they all point to the same underlying issue: your systems aren’t integrated in a way that supports how modern healthcare actually works.
And here’s the bottom line — integration is no longer optional, it’s foundational. The organizations that continue to operate with disconnected, siloed systems will find themselves falling behind, struggling with inefficiencies, losing revenue, frustrating their staff, and ultimately delivering a lower standard of care.
On the flip side, those that prioritize custom EHR integration are setting themselves up for smoother operations, better patient outcomes, and a technology infrastructure that can actually keep pace with the demands of modern medicine.
So if any of these signs resonated with you, take it as a nudge — not to panic, but to act. Start by evaluating your current systems honestly. Where are the gaps? Where is data getting stuck? Where are your teams spending time on workarounds that shouldn’t be necessary? Those are your starting points.
Custom EHR integration isn’t a one-size-fits-all solution, and it doesn’t happen overnight. But with the right strategy, the right partners, and a clear understanding of where your organization needs to go, it can be the single most impactful investment you make in your healthcare technology ecosystem. The signs are there. The question is — are you ready to act on them?
Want to assess your integration readiness? Then book your consultation right away.
FAQs
- What are the signs that a healthcare organization needs EHR integration?
There are several clear signs you need EHR integration in your organization. These include frequent data silos between systems, manual data entry errors, delayed access to patient records, lack of real-time communication between departments, and inefficiencies in billing or reporting. If clinicians are spending more time navigating systems than treating patients, it’s a strong indicator that robust EHR integration solutions are required to streamline workflows and improve care delivery.
- How does custom EHR integration improve clinical workflows?
Custom EHR integration significantly enhances clinical workflows by enabling seamless healthcare data integration across systems such as labs, pharmacies, and radiology. It eliminates redundant data entry, ensures real-time access to patient information, and automates routine tasks. One of the key custom EHR integration benefits is improved care coordination, allowing providers to make faster, data-driven decisions while reducing administrative burden.
- What are the benefits of integrating EHR with billing systems?
Integrating EHR with billing systems helps automate charge capture, reduce claim errors, and accelerate reimbursement cycles. Among the major benefits of custom EHR integration in healthcare is the ability to synchronize clinical documentation with billing workflows, ensuring accuracy and compliance. This type of EHR integration solutions also improves revenue cycle management by minimizing coding discrepancies and enhancing financial transparency.
- Is custom EHR integration suitable for small clinics?
Yes, custom EHR integration is highly suitable for small clinics. In fact, smaller practices can gain significant value from tailored EHR integration solutions that align with their specific workflows and budget constraints. The custom EHR integration benefits for small clinics include improved efficiency, better patient data accessibility, and scalability as the practice grows—without the complexity of large, off-the-shelf systems.
- How does FHIR support healthcare interoperability?
HL7 FHIR integration plays a critical role in modern interoperability by enabling standardized, API-driven data exchange between healthcare systems. FHIR allows different applications to communicate using structured formats, making healthcare data integration faster, more flexible, and scalable. It supports real-time data sharing, which is essential for connected care ecosystems and patient-centered healthcare delivery.
- What challenges can arise without proper EHR integration?
Without proper integration, healthcare organizations face fragmented data, increased administrative workload, higher risk of medical errors, and poor care coordination. These challenges highlight the signs you need EHR integration, especially when systems fail to communicate effectively. Lack of reliable EHR integration solutions can also lead to compliance risks, inefficiencies in operations, and reduced patient satisfaction.
- How long does it take to implement EHR integration?
The timeline for implementing EHR integration varies depending on system complexity, number of integrations, and data migration requirements. On average, it can take anywhere from a few weeks to several months. Advanced EHR integration solutions, especially those involving HL7 FHIR integration, may require additional time for customization, testing, and compliance validation to ensure seamless healthcare data integration.
- Which systems can be integrated with an EHR?
EHR systems can be integrated with a wide range of healthcare and administrative systems, including laboratory information systems (LIS), radiology systems (RIS/PACS), pharmacy systems, billing and revenue cycle management tools, telehealth platforms, and remote patient monitoring devices. These EHR integration solutions enable comprehensive healthcare data integration, ensuring a unified view of patient information and unlocking the full benefits of custom EHR integration in healthcare.